Now live! RTHM Direct – simplified medication access for Long COVID, ME/CFS and related conditions. Check it out
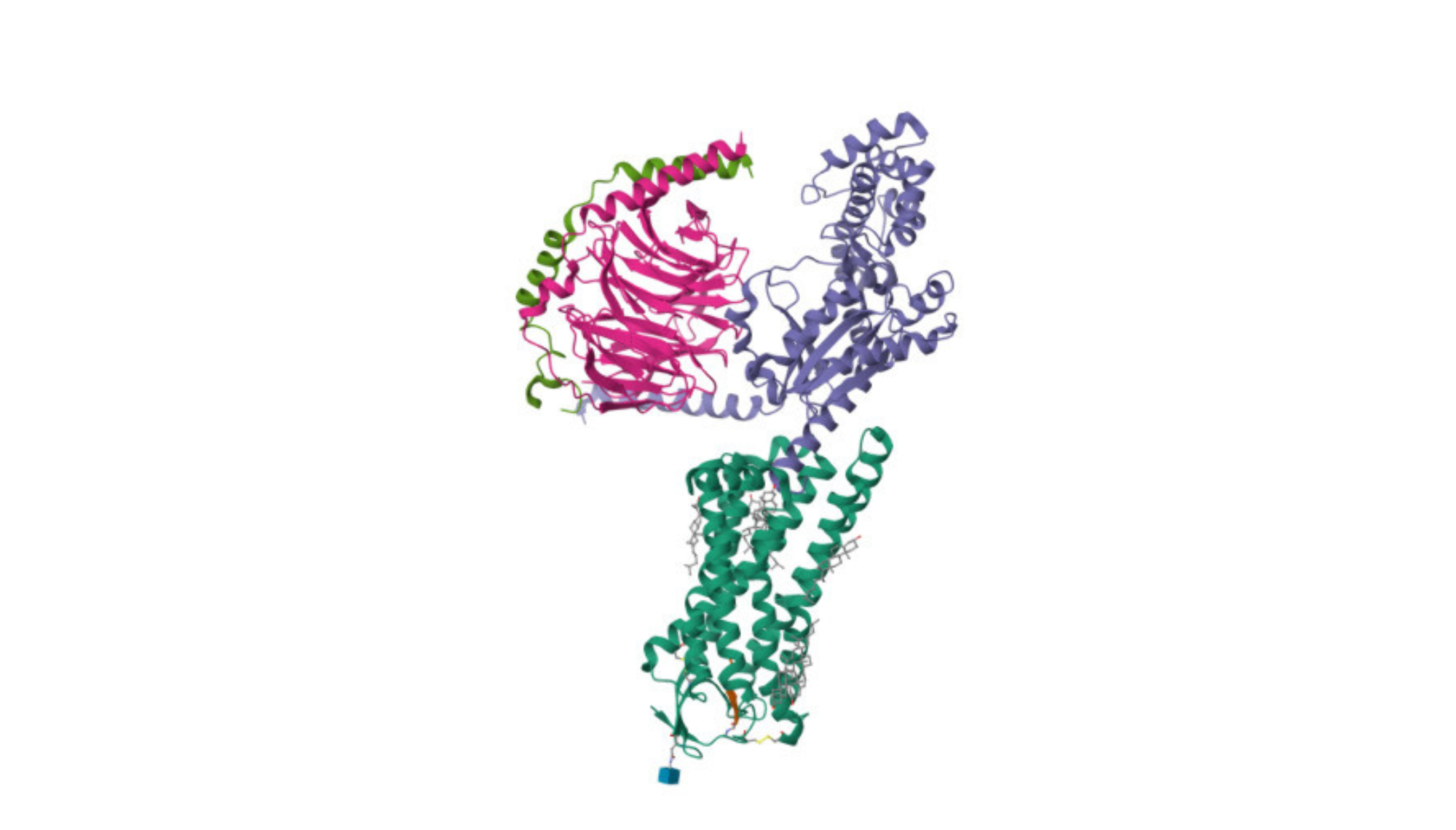
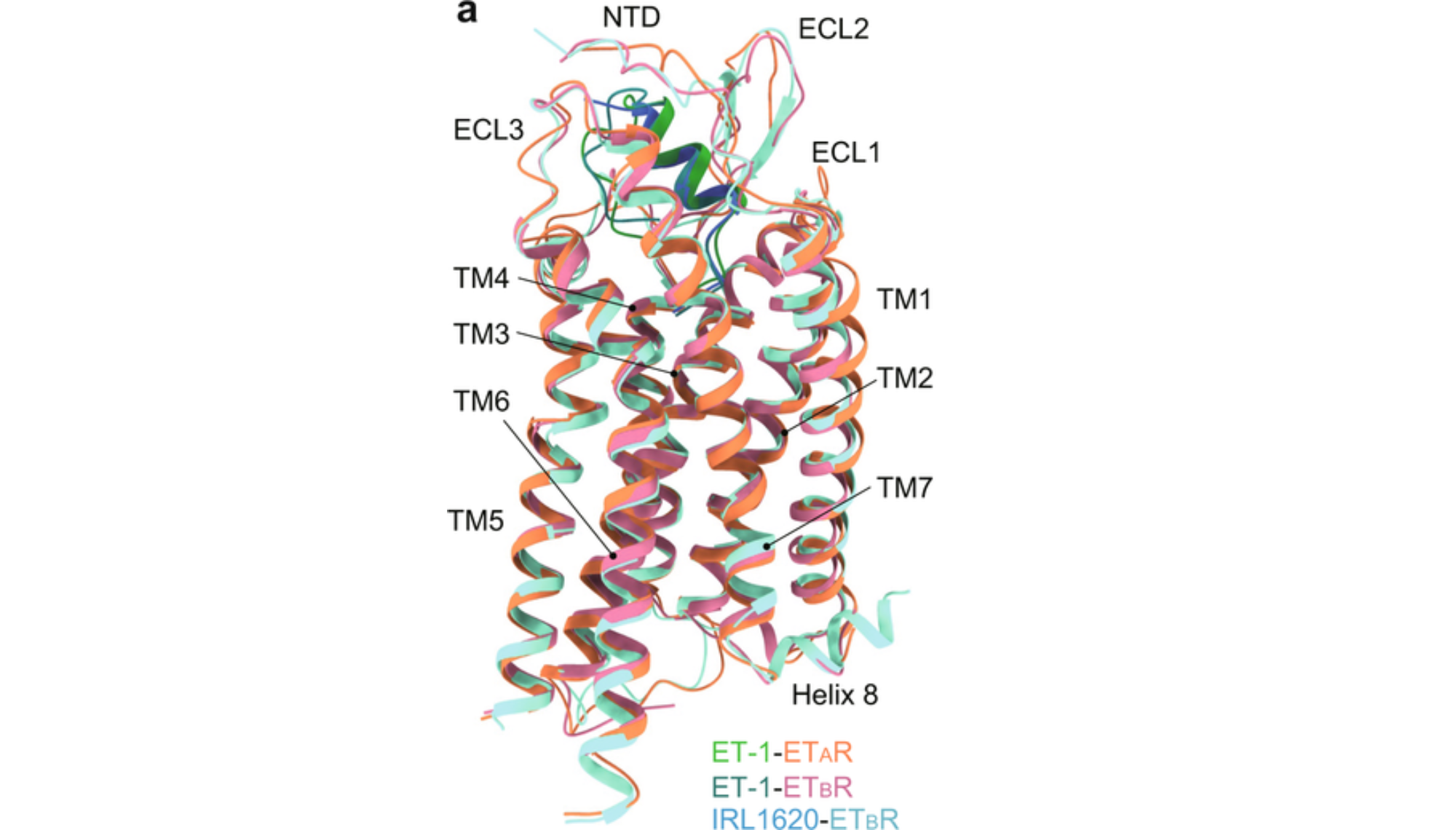
The α1 Adrenergic Receptor Autoantibody (α1-AR) is a G protein-coupled receptor. The α1-AR plays a crucial role in mediating vasoconstriction in response to catecholamines, thereby influencing blood pressure and vascular tone. The receptor consists of three homologous subtypes, including α1A-, α1B-, and α1D-adrenergic. Catecholamines like norepinephrine (noradrenaline) and epinephrine (adrenaline) signal through the α1-adrenergic receptors in the central and peripheral nervous system. The downstream second messenger mechanism for the α1-adrenergic receptor (α1-AR) involves the activation of the phospholipase C (PLC) pathway leading to the release of calcium ions (Ca2+) from intracellular stores. The increase in intracellular calcium and activation of PKC contribute to the physiological effects of α1-AR activation.
Functions of the α1 Adrenergic Receptor (α1-AR)
The functions of the α1 Adrenergic Receptor AAb (α1-AR) include:
- Vasoconstriction: Activation of the α1 Adrenergic Receptor on smooth muscle cells in blood vessels leads to vasoconstriction, which narrows the blood vessels and increases blood pressure.
- Pupil Dilation: Stimulation of the α1 Adrenergic Receptor in the iris dilates the pupil, allowing more light to enter the eye.
- Smooth Muscle Contraction: Activation of the α1 Adrenergic Receptor in various smooth muscle tissues, such as the bladder, prostate, and gastrointestinal tract, causes contraction and increased muscle tone.
- Glycogenolysis: The α1 Adrenergic Receptor plays a role in the breakdown of glycogen into glucose in the liver, leading to an increase in blood glucose levels.
- Inhibition of Insulin Secretion: Stimulation of the α1 Adrenergic Receptor inhibits insulin secretion from pancreatic beta cells, which helps to maintain blood glucose levels during times of stress or exercise.
- Modulation of Central Nervous System Activity: The α1 Adrenergic Receptor is also present in the central nervous system, where it modulates various functions, including sympathetic outflow and pain perception.
Please note that these functions may vary depending on the specific subtype of the α1 Adrenergic Receptor and the tissue or organ in which it is located. (Byund 19) (Andersen 1995) (Philipp et al. 2002)
Autoantibodies to α1 Adrenergic Receptor (α1-AR)
Autoantibodies against α1-adrenergic receptors have been found in various conditions, including prostate cancer, Alzheimer’s disease, vascular dementia, and hypertension. These autoantibodies can activate the receptors and trigger signaling pathways, leading to pathological effects. (Wallukat et al. 2020) (Karczewski et al. 2012) (Luther et al. 1997) (Hempel et al. 2017)
COVID-19 and Long COVID
There is evidence of the presence of autoantibodies against α1-adrenergic receptors in COVID-19 and Long COVID. These autoantibodies are part of a group of functional autoantibodies targeting G-protein-coupled receptors (GPCR-AAbs) that have been observed in patients after SARS-CoV-2 infection. Studies have shown that the seropositivity of GPCR-AAbs, including those targeting α1-adrenergic receptors, is associated with impaired retinal capillary microcirculation and other symptoms such as in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS) and loss of taste. Neutralizing these autoantibodies may improve the symptoms of Long COVID. (Szewczykowski et al. 2022)
Myalgic Encephalomyelitis/Chronic Fatigue Syndrome
There is limited evidence regarding the presence of autoantibodies against α1-adrenergic receptors in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS). However, one study “found that levels of α1/2- and beta1/2/3-AdR-, M3/4-AChR-, and AT1-R-, ETA/B-R-AAB/IgG ratios all significantly correlate with the severity of fatigue and, with the exception of beta3-AdR-AAB/IgG, with muscle pain. The severity of cognitive impairment correlated with AT1-R- and ETAR autoantibodies and the severity of gastrointestinal symptoms with α1/2-AdR-AAB.” (Freitag et al. 2021)
Dysautonomia and Postural Orthostatic Tachycardia Syndrome
There is evidence to suggest that autoantibodies against α1-adrenergic receptors may play a role in dysautonomia and postural orthostatic tachycardia syndrome (POTS). In a study examining patients with POTS, activating autoantibodies to the α1-adrenergic receptor were found in the serum of patients with POTS. These autoantibodies may contribute to the cardiovascular pathophysiological characteristics of POTS. However, it is important to note that the exact role of these autoantibodies in the development and progression of dysautonomia and POTS is still not fully understood, and further research is needed to elucidate their significance. (Yu et al. 2019) (Gunning et al. 2019) (Ruzieh et al. 2017) (Fedorowski et al. 2016) (Li et al. 2014)
Primary Hypertension
The autoantibodies may play a role in elevating peripheral vascular resistance and promoting cardiac hypertrophy, without exhibiting desensitization phenomena typically associated with receptor activation. (Luther et al. 1997)
Alzheimer’s Disease
A study suggests a potential role of α1-adrenergic receptor antibodies in Alzheimer’s disease, with improved function following Immunoabsorbance of the AAb’s. (Karczewski et al. 2018) Reduction in blood flow and the density of intact vessels was significantly demonstrated. The agAAB was removed through immunoadsorption in a small cohort of patients with Alzheimer’s disease. Subsequent follow-up observations over 12-18 months noted stabilization of cognition levels.
Arterial Stiffness Progression
In normotensive subjects, autoantibodies against α1-AR have been associated with the prediction of arterial stiffness progression over a 5-year period. (Li et al. 2017)
Hypertension Immunology
This study finds a correlation with hypertension, specifically with autoantibodies against AT1-receptor and α1-adrenergic receptors. The effects of the autoantibodies against α1-AR are proposed to contribute to pathogenesis. (Liao et al. 2002)
Preeclampsia
This is a complication of pregnancy characterized by high blood pressure and damage to another organ system, usually the liver and kidneys. There is evidence to suggest that autoantibodies against α1-adrenergic receptors (α1-ARs) may be present in preeclampsia. A study found that autoantibodies against α1-ARs were detected in women with severe preeclampsia. Another study also reported an association between the presence of autoantibodies against α1-ARs and severe preeclampsia. These autoantibodies may contribute to the pathogenesis of preeclampsia by activating α1-ARs and causing hypertension and other symptoms associated with the condition. However, more research is needed to fully understand the role of these autoantibodies in preeclampsia. (Ma et al. 2013)
Learn more about autoantibody testing at “RTHM Lab Now Offering GPCR+ Autoantibody Panel” and visit our Lab Page to order your GPCR+ Antibody Panel today.
Featured image courtesy of ThermoFisher Scientific.

Get updates
Join our mailing list