Endothelin A receptor (ETAR) autoantibody
September 14, 2025
AutoantibodiesETAR
Share:
Disclaimer: The information provided here is for educational purposes only and is not intended as medical advice. It should not be used to diagnose, treat, cure, or prevent any medical condition. Instead, use it as a starting point for discussion with your healthcare provider. Always consult with a qualified healthcare provider before starting any new medication, supplement, device, or making changes to your health regimen.
Endothelin Type-A Receptor AAb (ETAR) is a type of protein that belongs to the endothelin receptor group of G-protein-coupled receptors (GPCRs). This receptor is primarily located in the vascular smooth muscle. The ETAR primarily mediates vasoconstriction and cell proliferation in response to endothelin 1, playing a significant role in vascular tone and contributing to various cardiovascular and renal diseases.
Functions of the Endothelin Type A Receptor (ETAR)
ETAR, or Endothelin Type-A Receptor AAb (ETAR), is one of the receptors for endothelins, which are a family of potent vasoactive peptides. The main ligand for ETAR is endothelin-1 (ET-1), which is the most potent vasoconstrictor known. ETAR is a G-protein-coupled receptor (GPCR) that shares homology with the rhodopsin family of receptors. Like other GPCRs, ETAR is involved in signal transduction processes within cells, initiating a cascade of intracellular events upon activation by its ligands. (Hilal-Dandan and Brunton) Here’s a summary of its main functions:
Vasoconstriction: ET-1 binding to ETAR predominantly leads to vasoconstriction, which can result in an increase in blood pressure.
Cell Proliferation: Activation of the ETAR can lead to cell proliferation, especially in the vascular smooth muscle cells. This is significant in conditions like pulmonary arterial hypertension where excessive proliferation of the smooth muscle cells of the pulmonary arteries can lead to narrowing of the vessels.
Fibrosis: ETAR activation can also play a role in fibrosis in various tissues, including the heart and kidneys.
Release of Pro-inflammatory Mediators: This can further contribute to tissue damage and inflammation in various pathological states.
Cellular Expression: ETAR is expressed on both non-immune cells (like endothelial cells, vascular smooth muscle cells, and fibroblasts) and immune cells. This broad range of cellular expression suggests that ETAR has diverse functions within the body. (Kappes et al. 2020)
Ligand Selectivity: ETAR has particular ligand selectivity, distinguishing it from other endothelin receptors like Endothelin Type B Receptor (ETBR). This selectivity plays a crucial role in how ETAR contributes to various physiological and pathological processes. (Hilal-Dandan and Brunton)
Regulation of Blood Pressure and Kidney Function: ETAR, along with ETBR, is implicated in the regulation of kidney function and blood pressure. The interaction between endothelin receptors and other signaling molecules like dopamine may contribute to the maintenance of renal and cardiovascular homeostasis. (Pearl et al. 2020)
Involvement in Transplant Injury: There’s an increasing role of non-HLA antibodies targeting ETAR in humoral injury post-kidney transplantation, suggesting ETAR’s significance in transplant immunology and its potential impact on transplant outcomes. (Nowanska et al. 2021)
Endothelin System: ETAR is a part of the endothelin system which comprises two GPCRs (ETAR and ETBR) and three endogenous ligands (ET-1, ET-2, and ET-3). The endothelin system is integral to various physiological processes and is being studied for its role in several pathological conditions. (Horinouchi et al. 2013)
These functions and characteristics underline the importance of ETAR in maintaining cardiovascular homeostasis, kidney function, and potentially influencing outcomes in scenarios like organ transplantation.
Given these functions, antagonists of the ETAR (drugs that block its activity) are used therapeutically, particularly in conditions like pulmonary arterial hypertension. Bosentan is an example of a prescription drug that blocks both ETAR and ETBR (Endothelin Receptor Type B) and is used to treat pulmonary arterial hypertension. Blocking ETAR can lead to vasodilation and reduced cell proliferation, which are beneficial in this condition.
Autoantibodies to Endothelin Type-A Receptor (ETAR)
Autoantibodies against endothelin receptor A (ETAR) have been found in various medical conditions, including preeclampsia, benign prostatic hyperplasia, systemic lupus erythematosus-associated pulmonary arterial hypertension, systemic sclerosis, and COVID-19. These autoantibodies can activate ETAR and affect signaling pathways, potentially contributing to the pathogenesis of these diseases. They have been associated with disease progression, severity, and adverse outcomes. They can induce cellular and systemic events associated with disease pathogenesis, including the production of proinflammatory cytokines, collagen production, and endothelial dysfunction. However, more research is needed to fully understand their role and implications in these conditions. (Wallukat et al. 2017) (Guo et al. 2015) (Avouac et al. 2016) (Riemekasten et al. 2011)
COVID-19 and Long COVID
Autoantibodies against Endothelin Type-A Receptor AAb (ETAR) have been found to be increased in COVID-19 patients. These autoantibodies are associated with severe disease and may contribute to endothelial dysfunction and vascular pathology in COVID-19. (Miedema et al. 2023) (Miedema et al. 2021)
Another study showed that autoantibodies against ETAR were associated with an impaired retinal microcirculation, which could potentially reflect systemic microcirculation abnormalities seen in Long COVID. (Szewczykowski et al. 2022)
Dysautonomia and Myalgic Encephalomyelitis/Chronic Fatigue Syndrome
There is limited evidence regarding the association between autoantibodies against endothelin receptor A (ETAR) and dysautonomia. However, a study found that autoantibodies activating ETAR were associated with no-reflow (NR) in patients with ST-elevation myocardial infarction (STEMI), which is a condition involving impaired tissue perfusion. Another study investigated autoantibodies to vasoregulative G-protein-coupled receptors (including ETAR) in patients with myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) and found correlations between symptom severity and levels of these autoantibodies. While these studies provide some insights, further research is needed to fully understand the role of autoantibodies against ETAR in these conditions. (Tona et al. 2023) (Freitag et al. 2021)
Autoimmune Conditions
Autoantibodies against ETAR (Endothelin type A receptor) have been implicated in various autoimmune diseases. In systemic sclerosis (SSc), these autoantibodies have been found to play a role in the pathogenesis of the disease, contributing to the complex features of autoimmunity, inflammation, vasculopathy, and fibrosis. In primary Sjogren’s syndrome (pSS), decreased levels of autoantibodies against ETAR have been observed. Understanding the fluctuating levels of these autoantibodies helps researchers better map the progression of these complex autoimmune conditions and may eventually guide more targeted therapeutic approaches. (Akbarzadeh et al. 2023) (Yue et al. 2021)
Vascular Inflammation and Renal Function Decline
In pediatric kidney transplantation, antibodies against the Endothelin Type A Receptor are associated with Angiotensin II Type 1 Receptor antibodies, vascular inflammation, and a decline in renal function. Having both antibodies is significantly associated with arteritis, elevated IL-8, and a decline in renal function, and our results suggest possible interaction effects. These findings highlight the importance of monitoring autoantibody levels in transplant recipients. Early detection of these markers may help clinicians anticipate complications and adjust post-transplant care to better preserve kidney health. (Pearl et al. 2020)
Adverse Outcomes in Myocardial Interventions
Autoantibodies targeting ETAR can bind to the receptors and regulate their function. In cases of ST-segment elevation myocardial infarction (STEMI) following successful primary percutaneous coronary intervention, ETAR-autoantibodies may contribute to the no-reflow phenomenon, which is an undesirable outcome post-myocardial interventions. This phenomenon occurs when blood flow to the heart muscle remains impaired despite the reopening of the blocked artery. Recognizing the influence of ETAR-autoantibodies in this process could pave the way for novel strategies to improve recovery and cardiovascular outcomes in heart attack patients. (Tona et al. 2023)
Conclusion
These findings indicate that autoantibodies to the Endothelin Type-A Receptor have a multi-faceted impact on human health, particularly in the cardiovascular and renal systems, and may contribute to the pathogenesis of autoimmune diseases and adverse outcomes in cardiovascular interventions.
While RTHM is no longer offering direct testing, CellTrend will be able to provide information on how you can test today. Visit CellTrend.
As always, please consult with a qualified healthcare provider before making any changes to your treatment plan or if you have questions about autoantibody testing and your specific health needs.
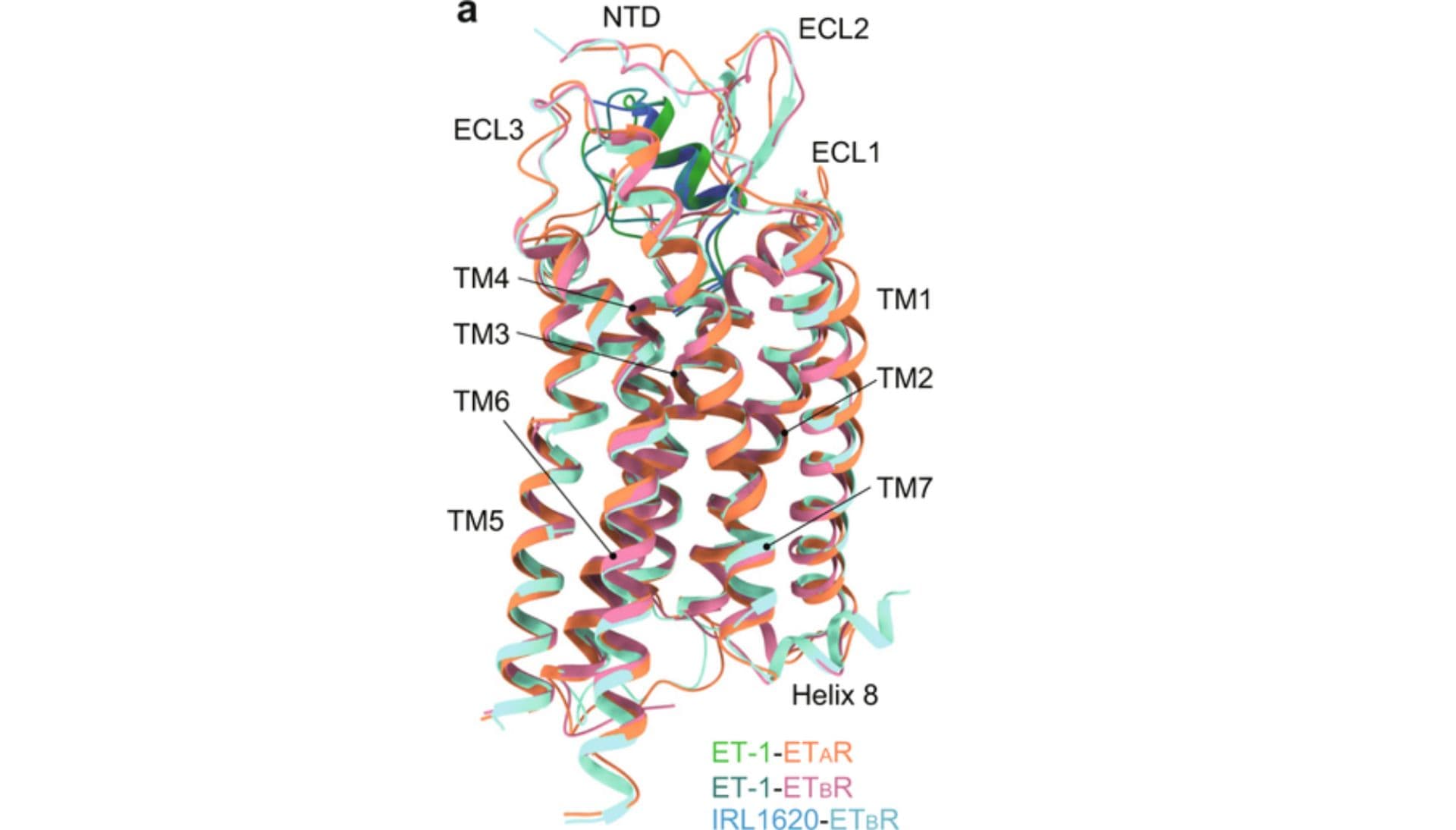
Featured image courtesy of Ji, Yujie & Duan, Jia & Yuan, Qingning & He, Xinheng & Yang, Gong & Zhu, Shengnan & Wu, Kai & Hu, Wen & Gao, Tianyu & Cheng, Xi & Jiang, H. & Xu, Eric & Jiang, Yi. (2023). Structural basis of peptide recognition and activation of endothelin receptors. Nature Communications. 14. DOI: 10.1038/s41467-023-36998-9.