Now live! RTHM Direct – simplified medication access for Long COVID, ME/CFS and related conditions. Check it out
In 1980, 108 million people worldwide were living with diabetes. By 2014, that number increased to 422 million and the International Diabetes Federation predicted in 2020 that an estimated 700 million adults worldwide will have diabetes in 2045. But that was before a connection was made between the SARS-CoV-2 virus and the increased incidence of newly diagnosed diabetes. In the United States, an American is diagnosed with diabetes every 17 seconds. But how will COVID affect these numbers and what does that mean in terms of the future? How is COVID changing the numbers when it comes to diabetes? What does this mean for healthcare in the future?
Diabetes and Acute COVID
When the COVID pandemic began, health officials announced a list of pre-existing conditions, such as cardiovascular disease, kidney disease, and obesity, that increased your risk for a more severe case of COVID. One of those risk factors was diabetes and growing evidence shows that a pre-existing diagnosis of diabetes greatly increases the risk of COVID severity, COVID-related mortality, and the development of Long COVID. For example, the Centers for Disease Control (CDC) shows that 40% of the COVID deaths early in the pandemic were in those with diabetes. Soebagijo Adi Soelistijo, an endocrinologist from the Indonesian Society of Internal Medicine, said that after the recent Omicron wave, the number of fatalities from COVID could be as high as seven times higher among those with diabetes than those with other pre-existing conditions.
SARS-CoV-2 Infection Triggering New-Onset Diabetes
Several studies have looked at the connection between COVID and diabetes since the start of the pandemic because it was considered a risk factor for severe acute infection. However, several studies are now finding that SARS-CoV-2 is contributing to a rise in new cases of diabetes.
How is SARS-COV-2 Causing Type I & II Diabetes?
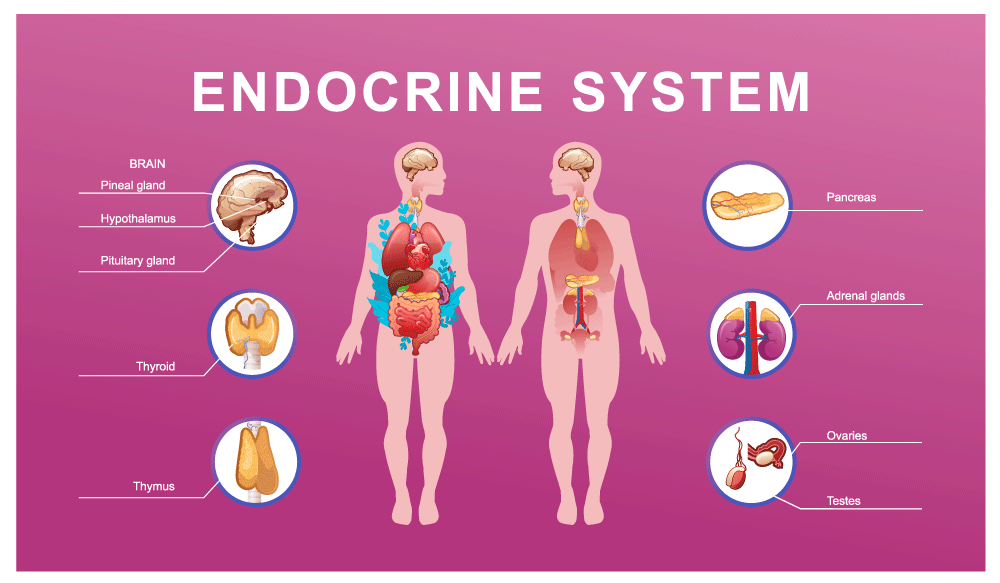
Researchers and physicians are seeing both an increase in type I and type II diabetes. Type I diabetes is a kind of autoimmune condition. In type I diabetes, the body attacks the cells in the pancreas, causing it to no longer produce insulin. In type II diabetes, the body still produces some insulin, though often not enough and when it does, other cells in the body do not respond to the insulin as they should.
When we look at type I diabetes and COVID, studies have shown that both transdifferentiation and cellular apoptosis can occur. In transdifferentiation, the SARS-CoV-2 virus infects human beta cells, the cells in the pancreas that secrete insulin. This alters their function, reducing the amount of insulin produced. Eventually, these cells no longer manufacture insulin. In cellular apoptosis, the virus kills the beta cells altogether, stopping the body’s ability to produce insulin.
Possible Underlying Causes
In most cases of type II diabetes, the underlying cause is typically obesity and an inactive lifestyle. When someone develops type II diabetes after COVID, there are some scenarios that could explain the new diagnosis.
- Pre-Diabetes
Over 38% of Americans (96 million people) over the age of 18 are considered prediabetic. This means they are at risk of diabetes. In many cases, they are unaware of this fact. In some cases, hospitalization for COVID finds the diagnosis or subsequent diagnosis of type II diabetes. - Undiagnosed Diabetes
It is estimated that 7.3 million adults in the United States are diabetic but undiagnosed. Treatment for COVID may have uncovered the diagnosis. - The COVID Pandemic
The lockdown and changes to healthy lifestyle routines may have led to the change from pre-diabetic to diabetic - Hormonal Changes in the Body
Recent work by Dr. James Lo from Weill Cornell Medicine suggests that spikes in blood sugar may be caused by low levels of the hormone in the body called adiponectin. This hormone, created in the fat cells, sensitizes other cells in the body to insulin, thus helping to regulate blood sugar. SARS-CoV-2, however, seems to cause fat cells to malfunction and reduce their production of adiponectin causing insulin resistance. Dysregulation in blood sugar is common in many infectious states.
Short-Term Diabetes from COVID
A new study led by Harvard Medical School researchers concluded that some of the newly diagnosed cases of diabetes may be a transitory condition related to the acute stress of the SARS-CoV-2 infection. They believe that some of the new cases are the result of a condition called stress hyperglycemia. Stress hyperglycemia occurs when an acute illness, such as COVID, causes a temporary spike in glucose levels. For these patients, while treatment may be necessary at the start, it is likely to resolve with time. This means that patients with new-onset diabetes requiring treatment should be monitored and followed closely to see how their condition changes.
Managing New Diabetes
If you are experiencing Long COVID symptoms, including newly diagnosed diabetes, it is important that you find a multidisciplinary team of medical professionals to address all of your Long COVID symptoms and help manage your blood sugar levels. At RTHM, our multi-disciplinary team of specialists focuses on every aspect of your health, with the goal of helping you achieve a better quality of life that allows you to move forward. To learn more about how RTHM can help, contact us today.

Get updates
Join our mailing list