Now live! RTHM Direct – simplified medication access for Long COVID, ME/CFS and related conditions. Check it out
At the beginning of the COVID-19 pandemic, it appeared that the SARS-CoV-2 virus primarily attacked the respiratory system. However, as the virus continues to mutate and infect people around the world, researchers have learned that this virus affects multiple systems throughout the body, including the endocrine system. As the virus infects cells throughout the body, it is damaging these systems and leaving behind long-term dysregulation. This endocrine system dysregulation is leading to some of the widespread symptoms experienced by those with Long COVID.
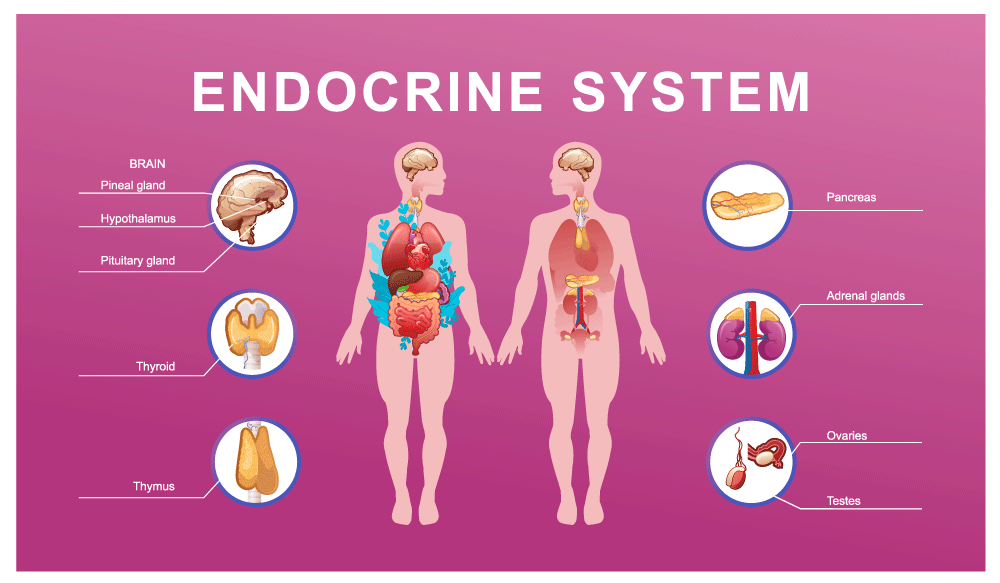
What is the Endocrine System?
The endocrine system is made up of glands that make and release hormones throughout the body. These hormones work as chemical messengers within the body, carrying information from one cell to another. These hormones play a role in many areas of your body and general health. This includes mood regulation, growth and development, organ function, metabolism, and reproduction. When even one of these hormones is out of balance, it can affect many areas of your overall health. These endocrine glands each have a different and specific role and are found throughout the body. To better understand the endocrine system, we can look specifically at each gland within the system.
Hypothalamus
Located in the lower part of the brain, the hypothalamus works as a link between the endocrine and nervous systems. Nerve cells within the hypothalamus collect information from the brain and send signals to the pituitary gland to release certain hormones it produces. This interaction helps control things like body temperature, thirst, hunger, sleep cycles, and emotional responses.
Pituitary gland
The pituitary gland is a small pea-sized gland at the base of the brain. It is considered the master conductor of the endocrine system. It receives information from the hypothalamus and then sends out hormones that communicate instructions to the other endocrine glands. The pituitary gland sends out a variety of hormones, such as:
- Antidiuretic hormone (ADH) – This hormone helps to control the water balance in your body as well as blood pressure regulation.
- Growth hormones – These hormones help stimulate bone and cell growth, as well as orchestrate how the body uses nutrients and minerals.
- Prolactin – This hormone is responsible for the production of milk for breastfeeding.
- Thyroid-stimulating hormone (TSH)– This stimulates the thyroid gland to produce thyroid hormones.
- Corticotropin – This stimulates the adrenal glands to create hormones.
- Oxytocin – This hormone triggers contractions during labor.
- Endorphins – These chemicals target the nervous system and help reduce feelings of pain.
Each hormone may have multiple jobs that affect multiple organ systems, and their interactions may be complex. In addition to these hormones, the pituitary gland is also responsible for controlling ovulation and menstrual cycle in women, as well as secreting hormones that trigger the reproductive organs to make estrogen and testosterone.
Thyroid
The thyroid is in your neck and produces the hormones thyroxine and triiodothyronine. These hormones regulate the rate at which cells convert the fuel from what you eat into energy, thus affecting growth and metabolism. When production of these hormones is low, you experience hypothyroidism which can cause heart rate reduction, loss of energy, and weight gain. On the other hand, when the thyroid makes too much of these hormones, known as hyperthyroidism, you may experience a jump in heart rate and unexplained weight loss.
Parathyroids
The parathyroids are four small glands that sit behind the thyroid. Their main function in the body is to maintain the levels of calcium and phosphorus in the body in order to regulate bone health.
Adrenal glands
The adrenal glands are located on the top of each kidney and the hormones they release control how the body responds to stress. Known for making the “fight or flight” hormones epinephrine (adrenaline) and norepinephrine (noradrenaline), these hormones can increase heart rate, increase blood flow, relax muscles, and help maintain blood pressure in response to stress. In addition to these hormones, the adrenal glands also produce cortisol. This hormone helps to regulate how your body uses fats, proteins, and carbohydrates. It also works to regulate blood pressure, increase blood sugar when needed, and suppress inflammation. Cortisol also plays a role in your sleep and wake cycle. Other hormones produced by the adrenal glands include aldosterone and DHEA.
Pineal body
The pineal body is a small gland found in the brain and is responsible for the hormone melatonin that responds to darkness and helps establish your circadian rhythm or internal clock.
Pancreas
The pancreas plays a role in two different systems in the body: the digestive system and the endocrine system. In the digestive system, the pancreas produces enzymes that help to break down the food you eat. For the endocrine system, the pancreas makes insulin and glucagon that help regulate the amount of sugar you have in your bloodstream. When your body does not make these hormones, your blood sugar becomes dangerously high, and you are diagnosed with Type I diabetes. If you still produce some of these hormones but not enough to regulate blood sugar, then you have Type II diabetes.
Thymus
The thymus also plays a role in two different systems: the endocrine system and the lymphatic system. This gland sits underneath the breastbone, between the lungs. The thymus is responsible for making T lymphocytes, or T cells, that play a major role in your immune system. The hormones released from the thymus help these T cells develop and keep the immune system functioning as it should.
Ovaries
In women, the ovaries produce estrogen and progesterone. These hormones help in development during puberty, regulate the menstrual cycle, and help support pregnancy.
Testes
In men, the testes produce testosterone. This hormone helps regulate everything from sex drive and sperm production to bone mass, muscle mass, and fat distribution.
Common Endocrine and Metabolic Conditions
Endocrine disorders occur when the glands within the endocrine system produce too much of a specific hormone, do not produce enough of a specific hormone, or your body does not respond to the hormones as they should. This creates a hormonal imbalance and can affect multiple areas of the body. This change in hormone production can occur as the result of a genetic disorder, an infection, tumors, or an injury to the specific endocrine gland.
Some common endocrine disorders include:
- Type I Diabetes – This occurs when damage to the pancreas and the insulin-producing cells stops the body’s ability to produce insulin.
- Type II Diabetes – The body’s cells become resistant to the action of insulin and the pancreas is unable to increase insulin production to overcome this resistance.
- Addison’s Disease – Damage to the adrenal gland reduces the amount of cortisol and aldosterone. This is the most common form of adrenal insufficiency.
- Cushing’s Syndrome – This occurs when the adrenal glands produce too much cortisol.
- Hyperthyroidism – This occurs when the thyroid becomes overactive and produces excess thyroid hormones. A common form of hyperthyroidism is Grave’s disease.
- Hypothyroidism – This occurs when the thyroid is underproductive and produces too little thyroid hormones. A common form of hypothyroidism is Hashimoto’s thyroiditis, or autoimmune thyroiditis.
How Does SARS-CoV-2 Affect the Endocrine System?
The connection between the endocrine system and the SARS-CoV-2 virus began at the start of the pandemic. Researchers and clinicians saw that those with underlying endocrine conditions, such as diabetes, thyroid disease, obesity, and low vitamin D levels experienced a greater risk of COVID severity. As the pandemic continues, we have learned that the SARS-CoV-2 virus binds to the ACE2 receptors. This allows the virus to enter cells in the endocrine system. In addition to immunological and inflammatory damage from the initial acute SARS-CoV-2 infection, this combination is producing endocrine manifestations (either new conditions or worsening of previous symptoms) in those with Long COVID. But what does that really mean and who is at risk?
Endocrine and Metabolic Conditions Seen with Long COVID
As we learn more about the SARS-CoV-2 virus and the subsequent Long COVID condition, we are seeing that many are experiencing complications with the endocrine system as a part of what we know as Long COVID. While we are still learning the extent of potential endocrine damage, new research is showing that the virus has affected many of the different glands within the endocrine system, resulting in the manifestation of new conditions or the worsening of symptoms in those with pre-existing endocrine conditions.
Increased New Cases of Diabetes Type I & II
Studies have found that the SARS-CoV-2 virus can contribute to new onset diabetes after an initial infection. It is normal for an acute illness to trigger the immune system into producing antibodies to fight the infection. However, this production of antibodies can often create antibodies that attack healthy cells in the body and, in this case, the pancreas. This attack can then affect the ability to produce insulin, resulting in type I diabetes. In addition, this stressor to the body can also increase insulin resistance, leading to type II diabetes.
Unfortunately, this new-onset diabetes is not limited to adults. Researchers show that children have an increased risk of developing type 1 diabetes within 30 days of acute COVID disease. In addition, they are seeing an increased frequency and severity of diabetic ketoacidosis (DKA), where the body produces excessive ketones, making the blood acidic. This is a life-threatening condition.
Adrenal Insufficiency
In addition to the pancreas, we are seeing damage to the hypothalamic-pituitary-adrenal (HPA) axis. This refers to the complex balance and communication between these hormone-producing glands and their ability to work together to maintain healthy endocrine function. This damage is leading to decreased levels of plasma cortisol and ACTH levels, which are consistent with adrenal insufficiency. This adrenal insufficiency may explain some Long COVID patients’ symptoms of severe fatigue and cognitive issues, such as brain fog and confusion.
Thyroid Hormone Changes
We already know that viral diseases can contribute to thyroid complications and the SARS-CoV-2 virus is no different. Acute COVID illness can trigger non-thyroidal illness syndrome (NTIS), which causes a decrease in some thyroid hormones and is often seen in people with critical illness. In contrast, others can experience subacute thyroiditis, or thyroid inflammation. This condition is also common after a viral infection, especially after an upper respiratory infection such as COVID. Unlike NTIS which often occurs during the acute COVID infection, subacute thyroiditis may occur weeks after the initial infection. This condition can cause an initial surge of thyroid hormone production.
Both conditions can cause symptoms typically seen in those with Long COVID. Hyperthyroidism can cause rapid heart rate, heart palpitations, anxiety, increased appetite, and unexplained weight loss. Hypothyroidism can cause unexplained fatigue, weight gain, hoarseness, muscle weakness, puffiness in the face, and dry skin.
Including the Endocrine System in Long COVID Care
Long COVID is a condition that can affect many different systems within the body, including the endocrine system. For this reason, Long COVID care requires multi-disciplinary care to address all possible complications. At RTHM, we focus on treating every patient with this multidisciplinary approach to help improve your overall health and quality of life with Long COVID. By combining research with clinical care, we strive to provide up-to-date treatment options as we continue to learn more about this disease.

Get updates
Join our mailing list