Now live! RTHM Direct – simplified medication access for Long COVID, ME/CFS and related conditions. Check it out
When the COVID pandemic began, the SARS-CoV-2 virus was believed to be a respiratory virus. However, as the pandemic progressed we learned that many systems of the body may be affected, including the gastrointestinal (GI) system. In fact, many people with acute COVID experience gastrointestinal symptoms before the more widely-discussed symptoms such as fever or respiratory issues. Many only experience gastrointestinal symptoms during their acute COVID stage. When it comes to Long COVID, those that experienced GI symptoms during the acute infection are more likely to see gastrointestinal symptoms persist. However, many Long COVID patients experience new GI symptoms weeks after acute COVID recovery.
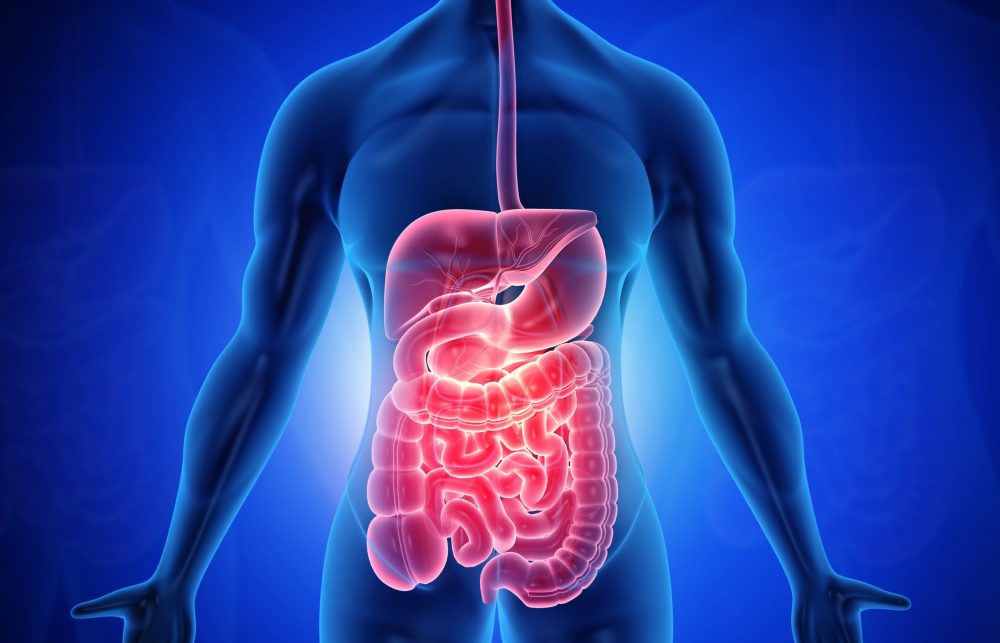
SARS-CoV-2 Can Damage the Gastrointestinal System During Acute Illness
The SARS-CoV-2 virus can affect the gastrointestinal tract in several ways. Some common damage seen during acute illness can include:
- Acute liver injury and elevated liver enzymes –
Elevated liver enzymes are common with acute COVID, but liver injury is typically mild. However, studies show that if severe liver injury occurs, it is more often seen with a more severe disease course. - Acute cholecystitis –
This occurs when the SARS-CoV-2 targets the ACE2 receptors in the GI system, which includes the gallbladder. - Acute pancreatitis –
This occurs when the SARS-CoV-2 targets the ACE2 receptors in the GI system, which includes the pancreas. - Ileus and feeding intolerance –
This occurs when the colon is unable to digest and move food and waste through the system. - Acute colonic pseudo-obstruction –
Also known as Ogilvie Syndrome, this condition affects the muscle contractions within the colon. - Mesenteric ischemia –
This is increased or blocked blood flow to the large or small intestines, often caused by blood clots.
Gastrointestinal Sequelae in Long COVID
Infection of the SARS-CoV-2 virus in the gastrointestinal system can disrupt the regular function of the gastrointestinal tract, with potential dysfunction showing up in the liver, pancreas, and gall bladder. This dysfunction can affect something as basic as the absorption of electrolytes and fluids. This damage can cause bleeding and blood clots in the gastrointestinal tract which can also restrict blood flow. Whether you experienced GI symptoms during your acute infection or not, you can still develop GI complications with Long COVID, and these symptoms can show up months after acute illness recovery.
Infection-associated GI issues are common after viral or bacterial infections and the SARS-CoV-2 virus seems to be no different. The most common infection-associated functional GI disorder is infection-associated irritable bowel syndrome (IBS) also known as infection-associated dysmotility. This is defined as the acute onset of IBS symptoms after an illness, such as a viral infection.
Common Long COVID Gastrointestinal Symptoms
Gastrointestinal symptoms associated with Long COVID can vary from person to person as well as in duration. You may experience a waxing and waning of symptoms, or they may become consistent and require additional testing. Some common GI symptoms can include:
- Nausea
- Vomiting
- Heartburn
- Diarrhea
- Constipation
- Abdominal bloating
- Change in appetite
- Acid reflux
- Upper abdominal pain
- GI bleeding
Symptoms That Require Immediate Attention
- Unexplained weight loss
- Difficulty swallowing
- Pain when swallowing
- Heartburn that wakes you up from sleep
- Nausea and vomiting every day
- Feeling full when eating much less
- Vomiting blood
- Blood in the stool
- Diarrhea in the middle of the night
- Fever
While traditional over-the-counter treatments are often enough to address most GI symptoms seen with Long COVID, if you continue to experience GI symptoms without any improvement, or experience any of the symptoms requiring attention above, testing with a gastroenterologist may be necessary to look for any other contributing factors.

Get updates
Join our mailing list