Muscarinic cholinergic receptor (M2R) autoantibody
September 14, 2025
AutoantibodiesM2R
Share:
Disclaimer: The information provided here is for educational purposes only and is not intended as medical advice. It should not be used to diagnose, treat, cure, or prevent any medical condition. Instead, use it as a starting point for discussion with your healthcare provider. Always consult with a qualified healthcare provider before starting any new medication, supplement, device, or making changes to your health regimen.
The M2 Muscarinic Receptor (M2-R or M2 mAChR) is primarily located in the heart, where its activation leads to a decrease in heart rate and cardiac contractility by inhibiting adenylate cyclase activity, thereby acting as a counter to the sympathetic nervous system’s stimulatory effects on the heart.
In more technical terms, M2 Muscarinic Receptors primarily couple to Gi/o proteins, which inhibit adenylate cyclase, leading to a decrease in cyclic AMP (cAMP) levels, which decreases heart rate and contractility (among other things). M2 receptors can also activate certain types of ion channels and trigger βγ-subunit signaling pathways.
Functions of the Muscarinic Cholinergic M2 Receptor (M2-R)
The M2 muscarinic receptor is one of the five muscarinic acetylcholine receptor subtypes (M1-M5). The M2 receptor, like other muscarinic receptors, is activated by the neurotransmitter acetylcholine. It is predominantly found in the heart and to a lesser extent in the central nervous system and other tissues. Below is a summary of its main functions.
However, first, let’s go over a little bit of heart anatomy. Below is an artistic depiction of the human heart showing its 4 main chambers: the left atrium, the right atrium, the left ventricle and the right ventricle.
Within the right atrium, is a cluster of cells called the sinoatrial (SA) node or the sinus node. These cells receive signals from the vagus nerve, sympathetic nerve fibers that modulate their spontaneous ability to “beat” and send a signal to the rest of the heart to do the same. The signal sent by the sinus node travels throughout the left and right atria (causing them to beat) first, pumping blood into the ventricles. That signal from the sinus node then reaches the atrioventricular (AV) node, which acts like a gatekeeper sitting just at the top of the muscular wall dividing the two ventricles of the heart. When the signal from the sinus node reaches the AV node, the AV node can let the signal pass through or block the signal from reaching the ventricles. In most cases, the AV node lets the signal from the sinus node pass through to the ventricles so that they then both contract, pumping blood from the left and right ventricles to the body and lungs respectively.
M2 mAChR Functions in the Heart
Decreased Heart Rate (Negative Chronotropy): Activation of M2 receptors in the sinus node within the upper right chamber of the heart (right atrium) slows down the heart rate.
Decreased Atrioventricular (AV) Node Conduction (Negative Dromotropy): M2 receptor stimulation in the AV node of the heart slows the conduction of electrical impulses from the top chambers of the heart (the atria) to the lower chambers of the heart (the ventricles)
Reduced Contractility in Atria (Negative Inotropy): Activation can decrease the force of atrial contraction, though the effect on the ventricles is less pronounced.
Central Nervous System
M2 receptors play roles in various central functions, including the modulation of dopaminergic neurotransmission, which is vital for motor control and reward pathways. Their specific roles in the central nervous system are complex and can vary significantly depending on the brain region. Research suggests they may also influence cognitive processes, memory consolidation, and pain perception by regulating the release of other neurotransmitters.
Smooth Muscle and Other Tissues
In some smooth muscle tissues, such as those found in the gastrointestinal tract and airways, M2 receptor activation can lead to muscle relaxation or modulate contractile responses. However, its presence and physiological significance vary widely across different tissues. For example, in the respiratory system, M2 receptors on nerve endings help limit the release of acetylcholine, thereby preventing excessive bronchoconstriction.
Presynaptic Inhibition
M2 receptors can be found presynaptically (on nerve terminals) where they function to inhibit the release of various neurotransmitters, including acetylcholine itself, acting as a feedback mechanism to modulate neurotransmission.
Given the critical role of M2 receptors in regulating heart rate and AV node conduction, drugs that act on these receptors or influence acetylcholine levels can significantly impact cardiac function. For instance, certain drugs that inhibit acetylcholine release or block its action can lead to an increased heart rate. Various drugs target M2 receptors to help manage conditions like heart arrhythmias and other cardiovascular diseases.
Autoantibodies to Muscarinic Cholinergic M2 Receptor (M2-R)
The strongest evidence linking M2-R autoantibodies to disease are for certain cardiovascular conditions, like arrhythmias. There is limited evidence that autoantibodies specifically against the M2-R are associated with postural orthostatic tachycardia syndrome (POTS), Long COVID, and ME/CFS.
Cardiac Arrhythmias
Circulating autoantibodies targeting M2 mAChR have been found in several cardiac arrhythmias. Elevated levels of these autoantibodies were identified in patients with atrial fibrillation (AF) and were positively associated with the recurrence of AF one year post-radiofrequency catheter ablation. (Ma et al. 2019)
Peripartum Cardiomyopathy (PPCM)
A study evaluated the impact of M2 mAChR autoantibodies on clinical outcomes in patients with PPCM undergoing standard treatment. The presence of these autoantibodies might affect the clinical outcomes in this patient group. (Ma et al. 2021)
Electrophysiological Effects
Autoantibodies against M2 mAChR are associated with electrophysiological changes, such as shortened action potential duration (APD), which might be a factor in atrial fibrillation in patients. This suggests that these autoantibodies could be one of the upstream targets of atrial fibrillation. (Baba et al. 2004)
Heart Rate Modulation
Functional autoantibodies directed to M2 mAChR could directly affect the heart rate by altering cardiac M2 mAChR activity and/or indirectly by changing vagal-mediated cardiac M2 mAChR activity. (Li et al. 2022)
These findings underline the possible pathological roles of autoantibodies against M2 muscarinic cholinergic receptors in various cardiac conditions. These findings also underscore the possible autoimmune connections in POTS and ME/CFS and the potential involvement of autoantibodies to muscarinic cholinergic receptors in the pathophysiology of these conditions.
Long COVID and Dysautonomia
There is limited evidence regarding the presence of autoantibodies to Muscarinic Cholinergic M2 Receptor (M2-R) in dysautonomia and postural orthostatic tachycardia syndrome (POTS). However, a study by Malkova and Shoenfeld (2022) discussed the imbalance of autoantibodies against G protein-coupled receptors (GPCR) in dysautonomia-related conditions. While they did not specifically mention M2-R autoantibodies, they highlighted the presence of autoantibodies against GPCR in autoimmune diseases and post-COVID syndrome. Additional studies found an association between muscarinic acetylcholine receptors and gastrointestinal symptoms and disease severity in those with POTS. Further research is needed to determine the role of M2-R autoantibodies in dysautonomia and POTS as well as a connection in those with Chagas disease and cardiovascular dysautonomia. (Malkova and Shoenfeld 2022) (Beltrame et al. 2020) (Sunami et al. 2022)
Evidence suggests that patients with POTS often have elevated levels of autoantibodies against adrenergic and muscarinic receptors, supporting the hypothesis that POTS may be an autoimmune disorder. (Gunning et al. 2019)
The presence of autoantibodies against adrenergic and cholinergic receptors, including muscarinic receptors, in patients with POTS and orthostatic hypotension has been identified. Higher titers of these antibodies correlate with the disease severity, and few reports have shown that immunomodulation therapy resulted in significant improvement in symptoms. (Ruzieh et al. 2017)
Myalgic Encephalomyelitis/Chronic Fatigue Syndrome
In ME/CFS patients, significant differences in anti-muscarinic cholinergic receptor 4 (anti-M4) antibody concentrations were found when compared to healthy donors. A consistent finding across ME/CFS, Herpes Simplex Encephalitis (HSE), and Long COVID is the development of autoimmune antibodies, which have been observed to have increased binding to adrenergic and muscarinic receptors, providing a window into neurocognitive disturbances, peripheral symptoms, POTS, and pain among other targets of these autoantibodies. (Bynke et al. 2020)
Testing and Additional Information
While RTHM is no longer offering direct testing, CellTrend will be able to provide information on how you can test today. Visit CellTrend.
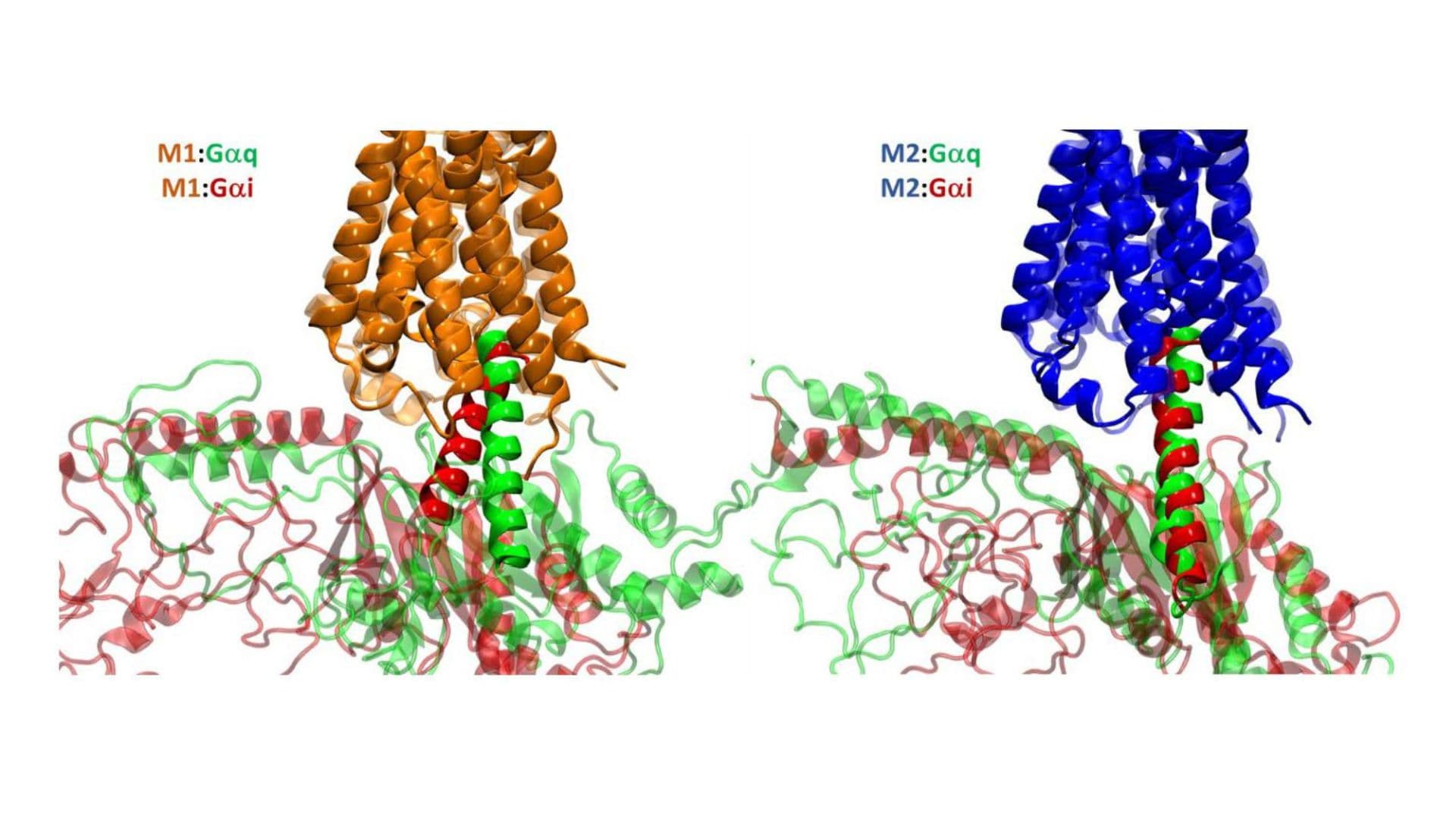
Featured image courtesy of Santiago LJ, Abrol R. Understanding G Protein Selectivity of Muscarinic Acetylcholine Receptors Using Computational Methods. International Journal of Molecular Sciences. 2019; 20(21):5290. https://doi.org/10.3390/ijms20215290
As always, please consult with a qualified healthcare provider before making any changes to your medical care or treatment plan.