Now live! RTHM Direct – simplified medication access for Long COVID, ME/CFS and related conditions. Check it out
ACE2 primarily serves as a counter-regulatory enzyme to the renin-angiotensin system (RAAS), converting angiotensin II to angiotensin-(1-7), thereby promoting vasodilation and reducing inflammation and fibrosis. Additionally, ACE2 is recognized as the primary receptor for the SARS-CoV-2 virus, the causative agent of COVID-19.
How is the ACE2 Different from the GPCRs in the GPCR+ Autoantibody Panel
Angiotensin-converting enzyme 2 (ACE2) and G protein-coupled receptors (GPCRs) are both membrane proteins but have different structures and functions.
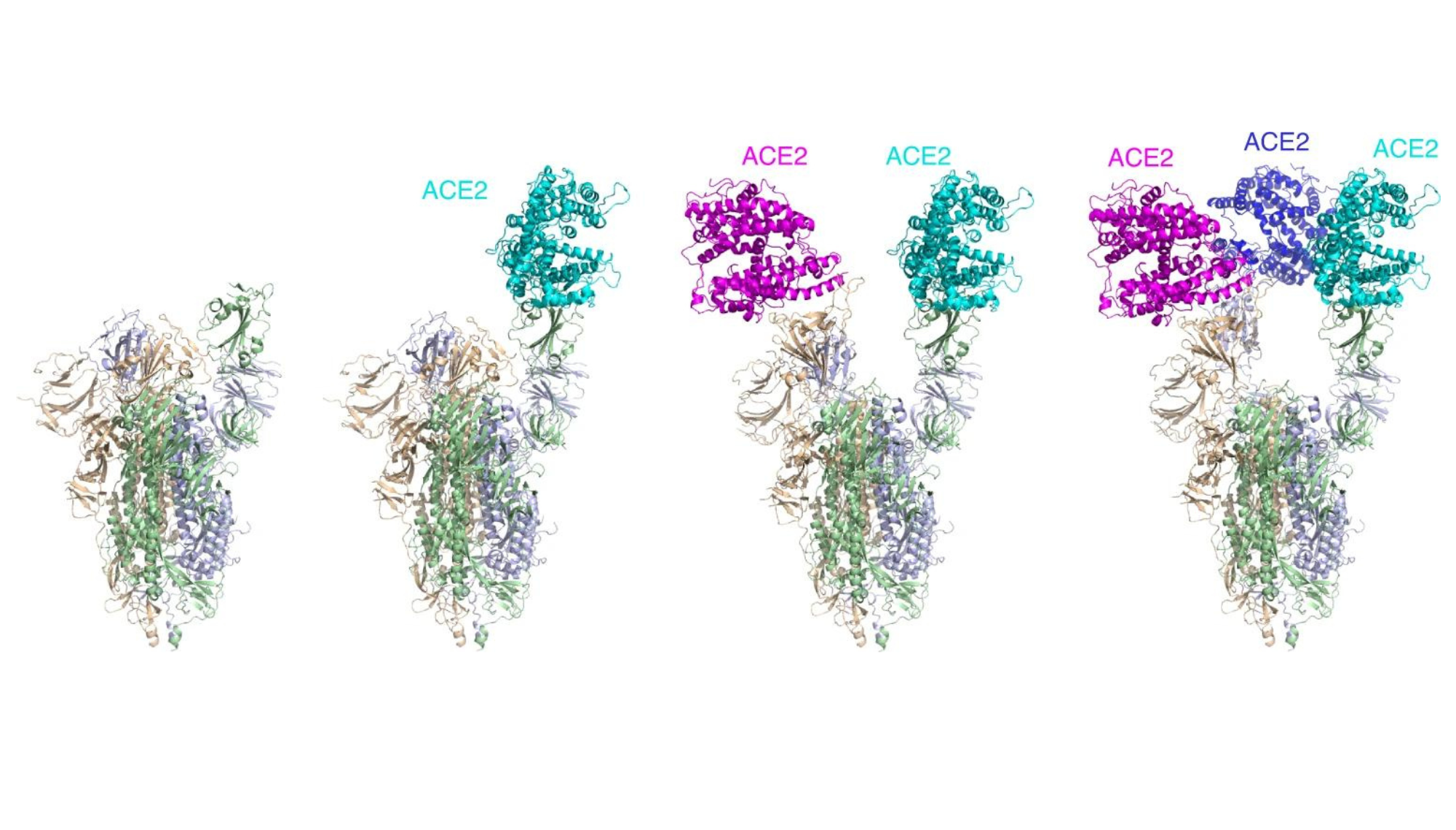
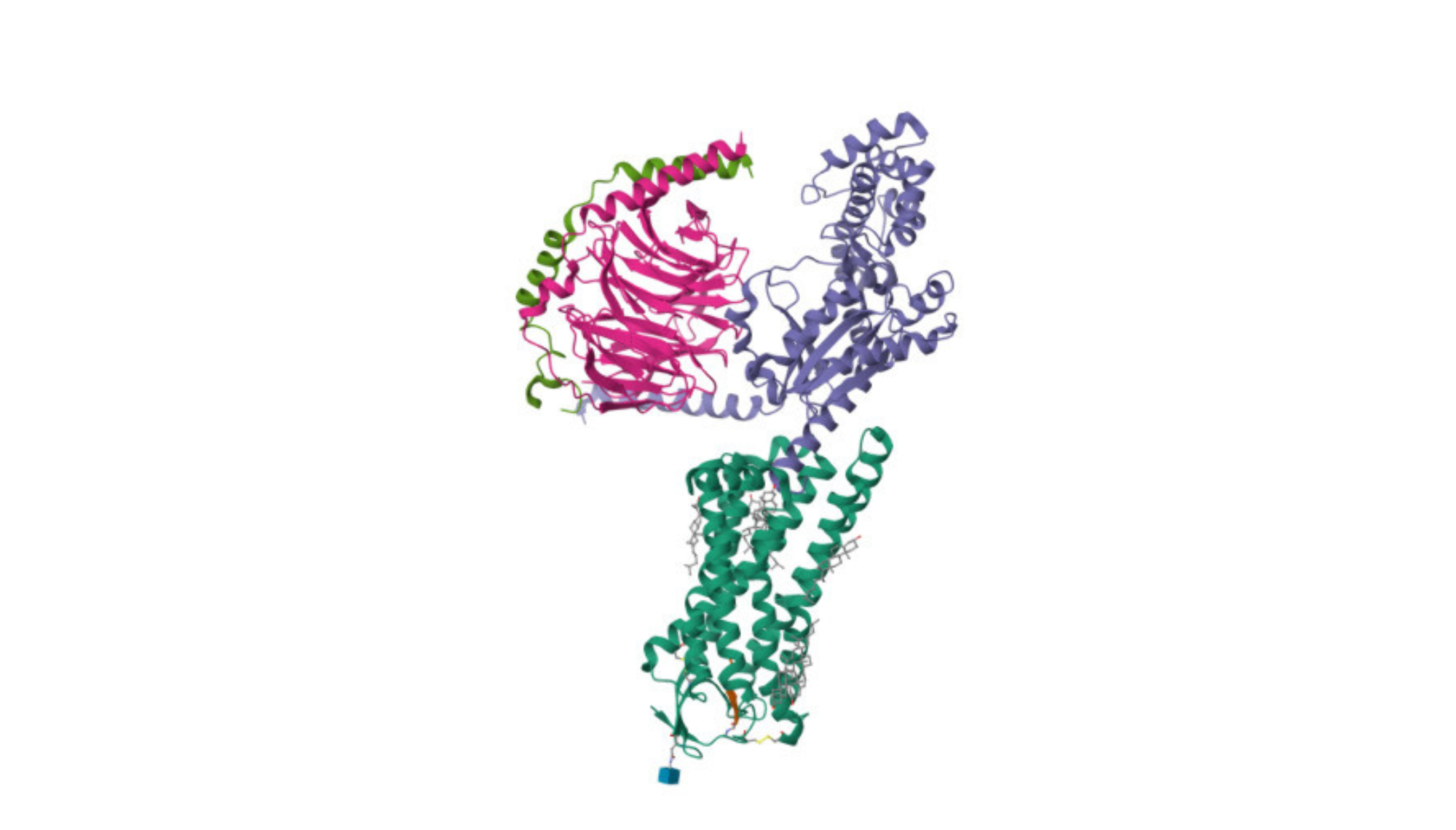
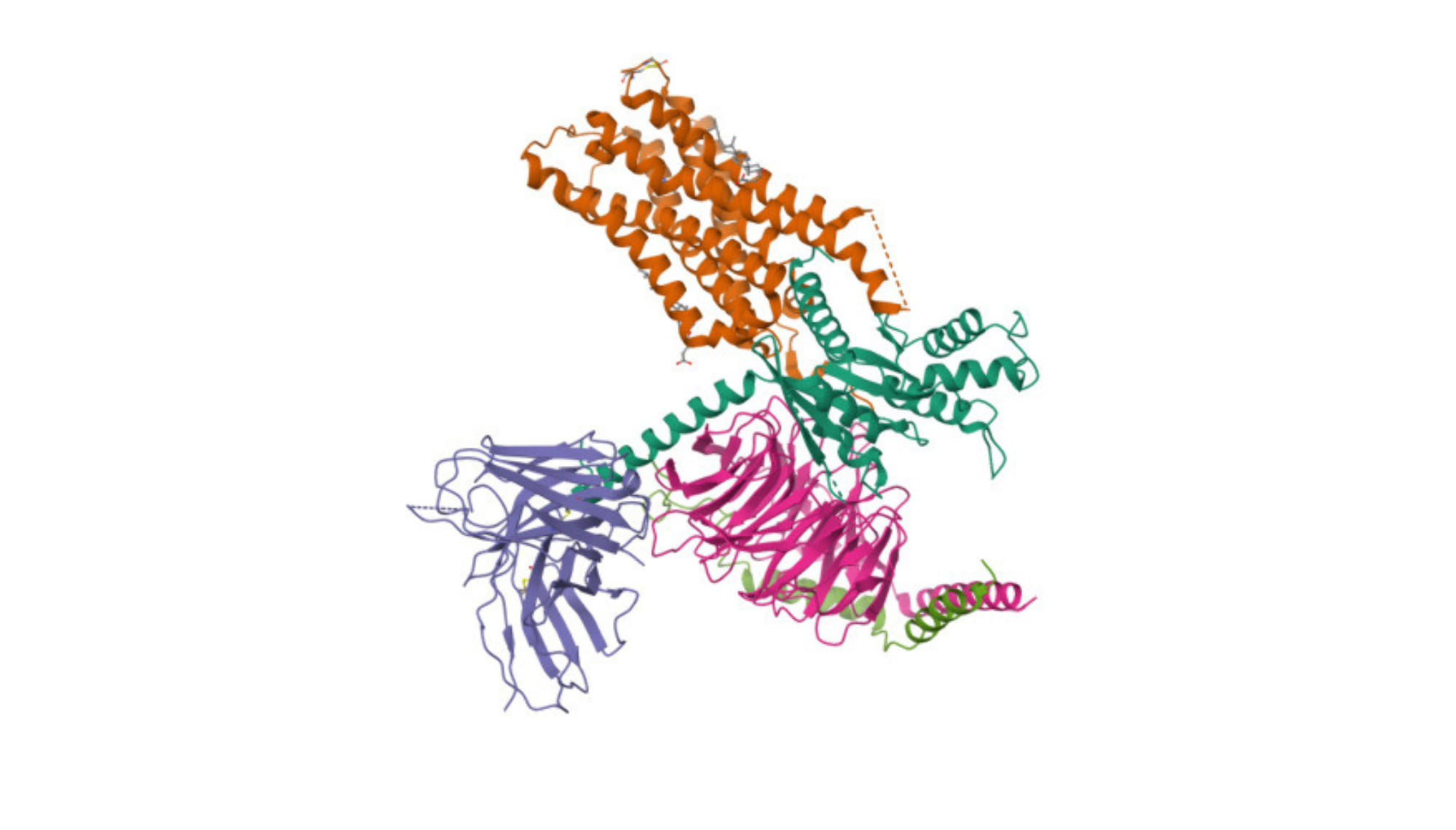
ACE2 is a type I transmembrane metallocarboxypeptidase with a single extracellular catalytic domain, which is responsible for its enzyme activity. It has a single membrane-spanning alpha-helix, with the majority of the enzyme projecting outside the cell. The extracellular domain is where the enzyme’s active site is located, and this is also the part of ACE2 that the SARS-CoV-2 virus’s spike protein binds to, facilitating viral entry into cells. Its structure is largely determined by its protein sequence and the requirements for the catalytic activity of the enzyme.
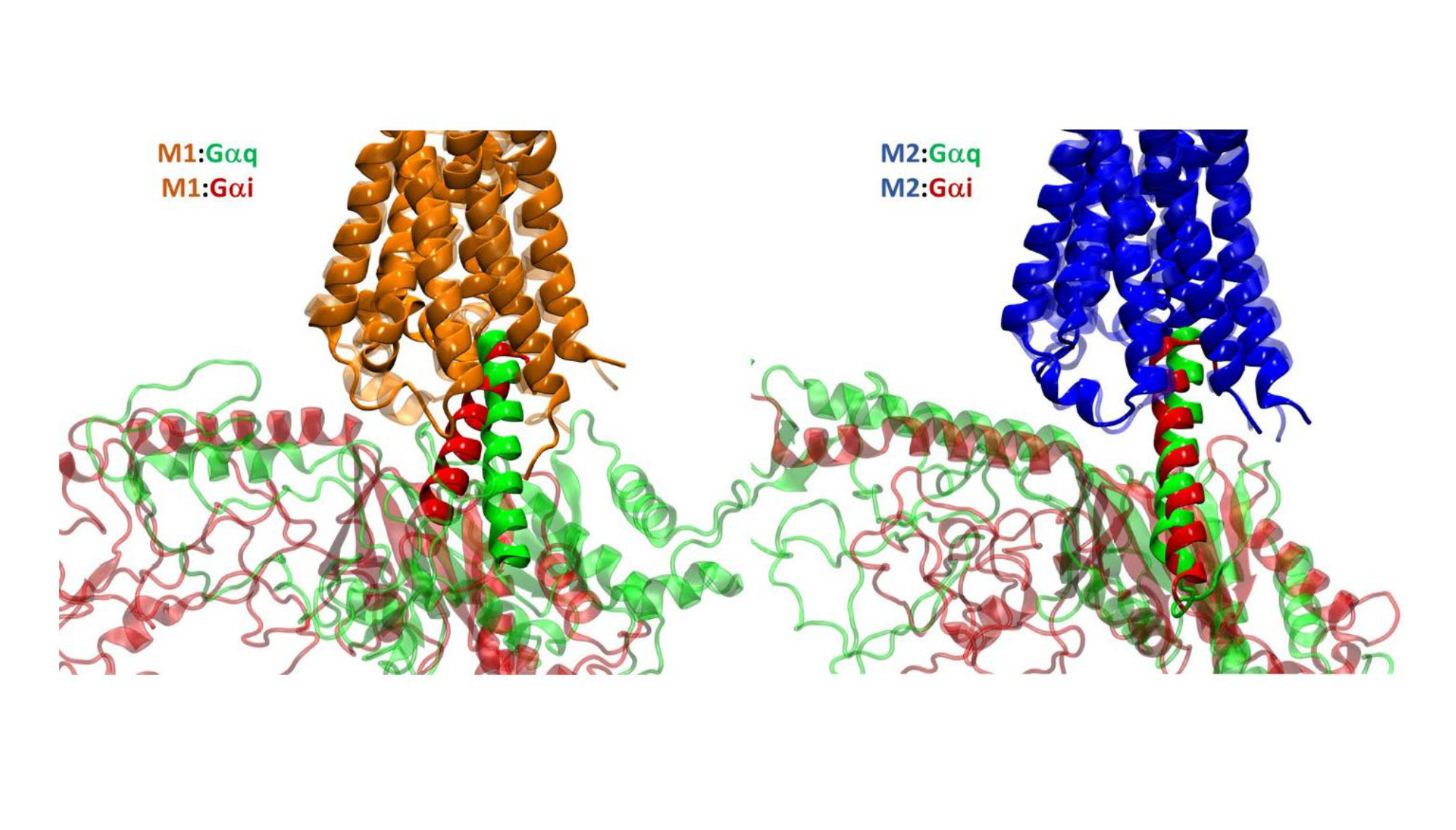
The main distinction is that ACE2 has a single transmembrane domain and acts as an enzyme, whereas GPCRs on the other hand have seven transmembrane domains and primarily act as signal transducers. They both interact with specific molecules, but they do so in very different ways and for different biological purposes.
Functions of the ACE2 Receptor
ACE2 stands for Angiotensin-Converting Enzyme 2. It’s a transmembrane protein mainly found in the lungs, heart, kidneys, and intestines. ACE2 plays a crucial role in the renin-angiotensin system (RAAS), a hormonal system that regulates blood pressure and fluid balance. Below is a summary of its main functions:
- Counterregulation of RAAS: ACE2 converts angiotensin II, a potent vasoconstrictor, into angiotensin-(1-7). Angiotensin-(1-7) generally exerts vasodilatory, anti-inflammatory, and anti-fibrotic effects, acting as a counterbalance to the classical RAAS pathway that promotes vasoconstriction and sodium retention.
- Protection in Organ Injury: The vasodilatory, anti-inflammatory, and anti-fibrotic effects of angiotensin-(1-7) have been found to be protective in models of heart, kidney, and lung injury.
- Balance in Blood Pressure Regulation: By converting angiotensin II into a molecule that promotes vasodilation (angiotensin-(1-7)), ACE2 helps to modulate blood pressure and counteract the hypertensive effects of the traditional RAAS pathway.
In addition to its physiological functions, ACE2 gained significant attention during the COVID-19 pandemic:
- SARS-CoV-2 Entry: ACE2 serves as the primary entry receptor for the SARS-CoV-2 virus, which is responsible for COVID-19. The virus binds via its spike protein to ACE2 in human cells, facilitating its entry and infection. This property has made ACE2 central to therapeutic investigations and considerations during the pandemic.
Given ACE2’s role in various physiological processes and its involvement in the COVID-19 pandemic, it has become an area of intensive research and interest in recent years.
Autoantibodies to ACE2 Receptor
Autoantibodies to the ACE2 Receptor AAb have been implicated in various diseases, including Parkinson’s disease and COVID-19. In Parkinson’s disease, autoantibodies against the angiotensin type-1 receptor (AT1R) and ACE2 have been found to be higher in patients and may contribute to disease progression. In COVID-19, autoantibodies against ACE2 have been detected in infected patients, and their presence may contribute to the long-lasting effects of the disease. These autoantibodies can activate complement, perturb vascular endothelial function, and impair blood pressure regulation. (Labandeira et al. 2022) (Hallmann et al. 2023)
Autoantibodies targeting the ACE-2 (Angiotensin-Converting Enzyme 2) Receptor have been investigated in various contexts, including post SARS-CoV-2 infection, and in patients with specific medical conditions like connective tissue diseases. Here are some of the noted effects and associations.

SARS-CoV-2 Infection and Long COVID
After SARS-CoV-2 infection, some patients develop autoantibodies against ACE2. These antibodies have been shown to decrease ACE2 activity, which could subsequently increase the levels of Angiotensin II (Ang II). Increased Ang II can trigger a proinflammatory state, potentially contributing to the symptoms of Post-Acute Sequelae after SARS-CoV-2 infection (PASC). (Arthur et al 2021)
A study found a significant positive correlation between serum levels of autoantibodies against ACE2 and a molecule called LIGHT (TNFSF14). This study suggests that these autoantibodies, by reducing the conversion of Angiotensin II, might be involved in certain mechanisms not directly related to COVID-19 severity. (Rodriguez-Perez et al. 2021)
There’s a hypothesis that delayed lung damage post-SARS-CoV-2 infection could be caused by an autoimmune response to ACE2. This is thought to occur due to the forced presentation of ACE2 protein in complex with the virus spike protein in certain cells in the lung, although the likelihood of this hypothesis being valid is considered low. (Townsend 2020)
Additional studies provide evidence of the association between COVID-19 and autoantibodies to ACE2. These autoantibodies have been found in patients with severe COVID-19 and are associated with disease severity. They can activate complement and contribute to the angiocentric pathology observed in some severe COVID-19 cases. However, more research is needed to fully understand the prevalence, effects, and potential therapeutic implications of these autoantibodies. (Casciola-Rosen et al. 2022) (Hallmann et al. 2023)
Parkinson’s Disease
In Parkinson’s disease, both angiotensin type-1 receptor (AT1) autoantibodies (AT1 agonists) and ACE2 autoantibodies (ACE2 antagonists) have been detected. These autoantibodies may play a role in disease progression and could potentially be targeted for therapeutic interventions. (Labandeira et al. 2022)
Connective Tissue Diseases
In patients with connective tissue diseases, a hypothesis was explored that serum autoantibodies to ACE2 might predispose them to constrictive vasculopathy, pulmonary arterial hypertension (PAH), or persistent digital ischemia. This is based on the role of ACE2 in converting Angiotensin II into Ang(1-7), which has vasoprotective effects. (Takahashi et al. 2010)
Learn more about autoantibody testing at “RTHM Lab Now Offering GPCR+ Autoantibody Panel” and visit our Lab Page to order your GPCR+ Antibody Panel today.
Featured Image courtesy of Xiao, T., Lu, J., Zhang, J. et al. A trimeric human angiotensin-converting enzyme 2 as an anti-SARS-CoV-2 agent. Nat Struct Mol Biol 28, 202–209 (2021). https://doi.org/10.1038/s41594-020-00549-3

Get updates
Join our mailing list